Raising the Bar with Intelligent Claims Management
Claims management systems process $1.5 trillion in claims annually. However, a massive 10% of claims payouts are leakage, resulting in an estimated $1.5 billion loss per annum for P&C insurers. This is largely down to the insurance industry’s dependence on legacy systems and manual processes, along with a lack of visibility into the claims process. So it’s no wonder that claims organizations are starting to see the value of claims intelligence, which creates efficiencies based on massive, centralized stores of data and reduces leakage that costs insurers far too much.
What is claims intelligence?
Intelligent claims management uses artificial intelligence (AI) and advanced claims technology to create personalized and contextual recommendations based on the insurer’s vast historical customer data as well as data collected during the claim process. For example, intelligent claims management can provide the adjuster with smart recommendations; automatically calculate the reserve; recommend the appropriate vendors; and take a lot of guesswork out of the claims process. This increases the efficiency of the claims process, results in significant savings, and improves the insurer’s decision making by creating process models based on data analysis.
Claims intelligence management can assist insurers in automating processes not requiring human intervention, e.g., assessing damage to properties following an event such as a hurricane by using visual intelligence from the Internet of Things (drone feeds, smart devices, etc.). UK insurer Brit used machine-learning algorithms and high-resolution aerial imagery to quickly and accurately identify Hurricane Ian property damage, issuing claims payments within days of the storm. Assessors can quickly make smarter decisions, shortening the claims process, reducing the cost of the process and increasing customer satisfaction.
How does claims intelligence work?
By implementing intelligent claims management software, insurers are empowered to make decisions backed by facts and context, resulting in a range of benefits, including:
- AI-based risk assessment enables insurers to more accurately customize plans and ensure they have the right reserves, while their customers pay only for what they actually need.
- AI and machine learning for automatic calculation of claims payouts, helping insurers significantly reduce claims leakage.
- Automated decision-making capabilities and prompts for quick claims resolution, increasing customer satisfaction and reducing client churn.
- AI detection of patterns that cannot be identified by humans, based on massive amounts of data, significantly reducing fraud and preventing major revenue losses.
Sounds great, but why is it so hard for insurers to adopt?
In theory, claims intelligence management is the solution all insurers have been waiting for. But, for many, it’s easier said than done. When you take a look at most insurers, their data is stored in multiple decentralized and disconnected databases. And that’s assuming that all data is stored, because ultimately not all customer data is saved for future use. But even the stored data is not always easy to locate and retrieve − it requires trained professionals to navigate a complex retrieval process that takes time. There’s no self-operation, there’s no real-time retrieval, and there’s no guarantee of finding all the required data.
Successful intelligent claims management can only be offered via a dedicated system that automatically and correctly stores all claims-related data in a centralized database ready for easy contextual retrieval and use, interfaces with other systems, and can be operated by the business owner in real time.
How do insurance companies use data to compile claims intelligence and use this information? For a closer look at the role data plays for insurance companies today and where claims intelligence is headed in the future, check out The State of Claims Intelligence 2022.
How is Five Sigma advancing claims intelligence?
With data at the heart of a claims operation it must be leveraged to increase efficiency, improve customer experience, and fuel future growth.
Five Sigma’s claims management solution (CMS) is a cloud-native, agile and scalable SaaS solution enabling insurers to automate their entire claims management process. It imports, collects, stores, and updates all data contextually, including all claims-related communication, in one database.
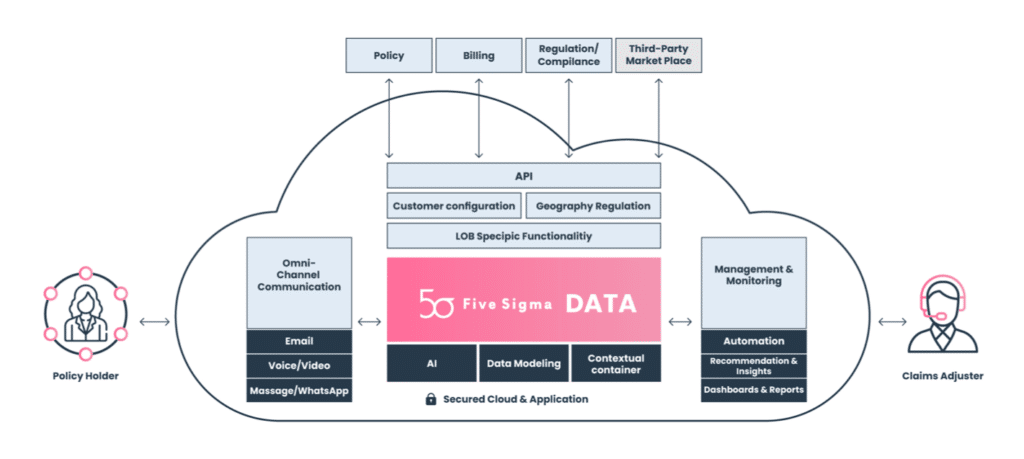
Five Sigma marketecture
The CMS uses historical and online data to generate personalized and contextual recommendations that help adjusters perform better. Complete visibility of data enables the generation of strategic insights that help insurers make smarter decisions to perfect their operations, sales processes, and more. Advanced API-based architecture enables integration with other applications and databases resulting in easy integration with policy administration, communication systems, and more.
Intelligent claims automation takes over tasks previously handled manually, such as filing or emailing reports, and enables adjusters to record and track their activities automatically, reducing human error. It streamlines communication by sending alerts, tasks, or messages to adjusters, improving communication and creating greater organizational competency.
The Five Sigma CMS is based on:
- Automation: Our proprietary workflows eliminate repetitive tasks, freeing your teams to focus on helping customers.
- AI for recommendations: Based on historical data, classification rules and AI methodologies, our system determines recommendations.
- Company-wide insights: Our claims data is used to build reports and dashboards, and our market knowledge base is used to understand and improve claims operations.
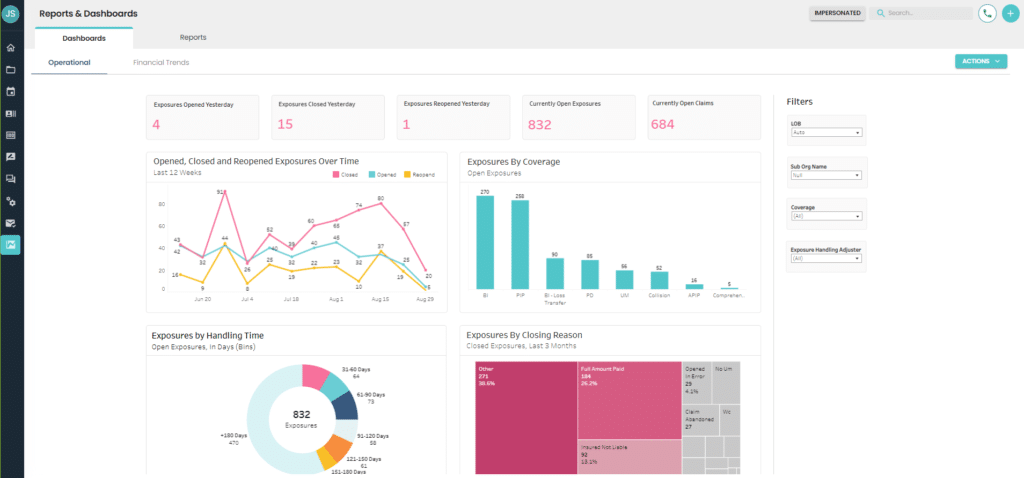
The Reports & Dashboards Module’s Operational dashboard
In order to make our data smart, accessible, and simple to use, our claims management solutions operate according to the following principles:
- Data centricity: We put data at the heart of everything and our system imports, collects, stores, and updates all data in one database.
- Data governance: Insurance applications collect a huge amount of data, however, in many cases, this data is not visible or accessible to the insurer. We make all claims data visible and accessible to the insurer at all times.
- Open platform/Data integration: Our API-based architecture enables us to easily integrate with other applications and databases, e.g., policy administration, communication systems, etc. We can also upload physical data using OCR technology and embed it into our database for future use.
- Time to market: Our claims management system is online and ready to address your needs anytime and anywhere.
- Self-operation: All data is accessible so that you can independently build and operate your own reports and dashboards directly from the cloud. The data is queryable and can be used for operation, monitoring, and management as well as historical snapshots.
Conclusion
Insurers seeking to increase their competitive edge understand the need to adopt intelligent claims management for increased efficiency, reduced leakage and customer retention. But insurers still relying on legacy systems that aren’t properly equipped to centrally store data, retrieve it in real time, or facilitate intelligent insights that will improve the claims process, can’t take advantage of the advances in intelligent claims management.
The solution lies in software that automates the collection, storage and contextual retrieval of all customer data from a centralized database, in real time, enabling intelligent automation of the claims process and reducing manual effort. Five Sigma’s claims management solution empowers insurers to automate their entire claims management process, gain actionable insights and recommendations based on AI, and improve their entire claims process.
Click here to request a demo of Five Sigma’s intelligent claims management solution, and see for yourself how it uses data to help your claims department maximize its efficiency and empower your claims adjusters.
Frequently Asked Questions
Why is claims management important?
Claims management processes all claim types, recognizes and pays out legitimate claims, accurately assesses the reserve associated with each claim, regularly reports on the claims process and minimizes costs, all while minimizing the time required to close the claim and avoid any legal consequences. Claims management calculates and processes complex recurring payments, and tracks each claim’s progress, while using best practices throughout the process. Claims management integrates with all relevant systems, such as policy administration in real-time, and provides adjusters with status reports.
How can claims management be improved?
Claims management can be significantly improved by implementing a dedicated intelligent claims management system that automatically and correctly stores all claims-related data in a centralized database ready for easy contextual retrieval and use, interfaces with other systems, and can be operated by the business owner in real time. An intelligent claims management system enables insurers to automate processes not requiring human intervention, for example, assessing damage to properties following an event such as a hurricane by using visual intelligence from the Internet of Things (drone feeds, smart devices, etc.). Assessors can quickly make smarter decisions, shortening the claims process, reducing the cost of the process and increasing customer satisfaction. Intelligent claims management systems automatically and correctly store all claims-related data in a centralized database ready for easy contextual retrieval and use, interface with other systems, and can be operated by the business owner in real time. Intelligent claims management enables insurers to make decisions based on vast centralized stores of customer data, backed by facts and context.

